Experiments show that an “unknown” enzyme fights inflammation
An enzyme that normally repairs damaged DNA may be the key to a new treatment for inflammatory diseases.
Inflammatory diseases such as COPD and septicemia (blood poisoning) represent a growing threat to public health. These conditions are commonly the result of an overactive immune system.
This is why the discovery of the drug candidate TH5487 has attracted so much attention. The molecule disarms a protein that appears to play a key role in inflammatory diseases, and experiments have shown that it suppresses lung inflammation in mice.
The discovery has been made by research scientists at the Karolinska Institute in Stockholm, Stockholm University, the University of Texas, and at NTNU and SINTEF in Trondheim, Norway. After a five-year research project, the results were published in the journal Science.
Key signal substance causes overactivity
Patients suffering from inflammatory diseases have large amounts of a signal substance in their bodies, known to biochemists as ROS. ROS is an abbreviation for “reactive oxygen species”, which triggers inflammation and damages the genetic material, DNA, in our cells.
“This damage is repaired by the enzyme OGG1. Our research shows that this ‘repair’ also acts as a trigger that promotes overactivity in the immune systems of those patients suffering from autoimmune diseases,” says Torkild Visnes, a SINTEF researcher.
“It may sound illogical, but in many diseases it is an overactive immune system that constitutes the problem,” he says.
This finding agrees with previous research showing that mice lacking the OGG1 enzyme are unable to activate a powerful immune response. As a result, these mice have milder inflammation than normal mice.
Painstaking study of 18,000 substances
“Our idea was to look for a chemical substance that would attach itself to the repair protein OGG1”, says Visnes. “This substance would then be used to ‘disarm’ the protein by persuading it to respond as if it had already found damaged DNA, and in doing so inhibit its activity. In other words, deprive the protein of its ability to trigger an overactive immune response.”
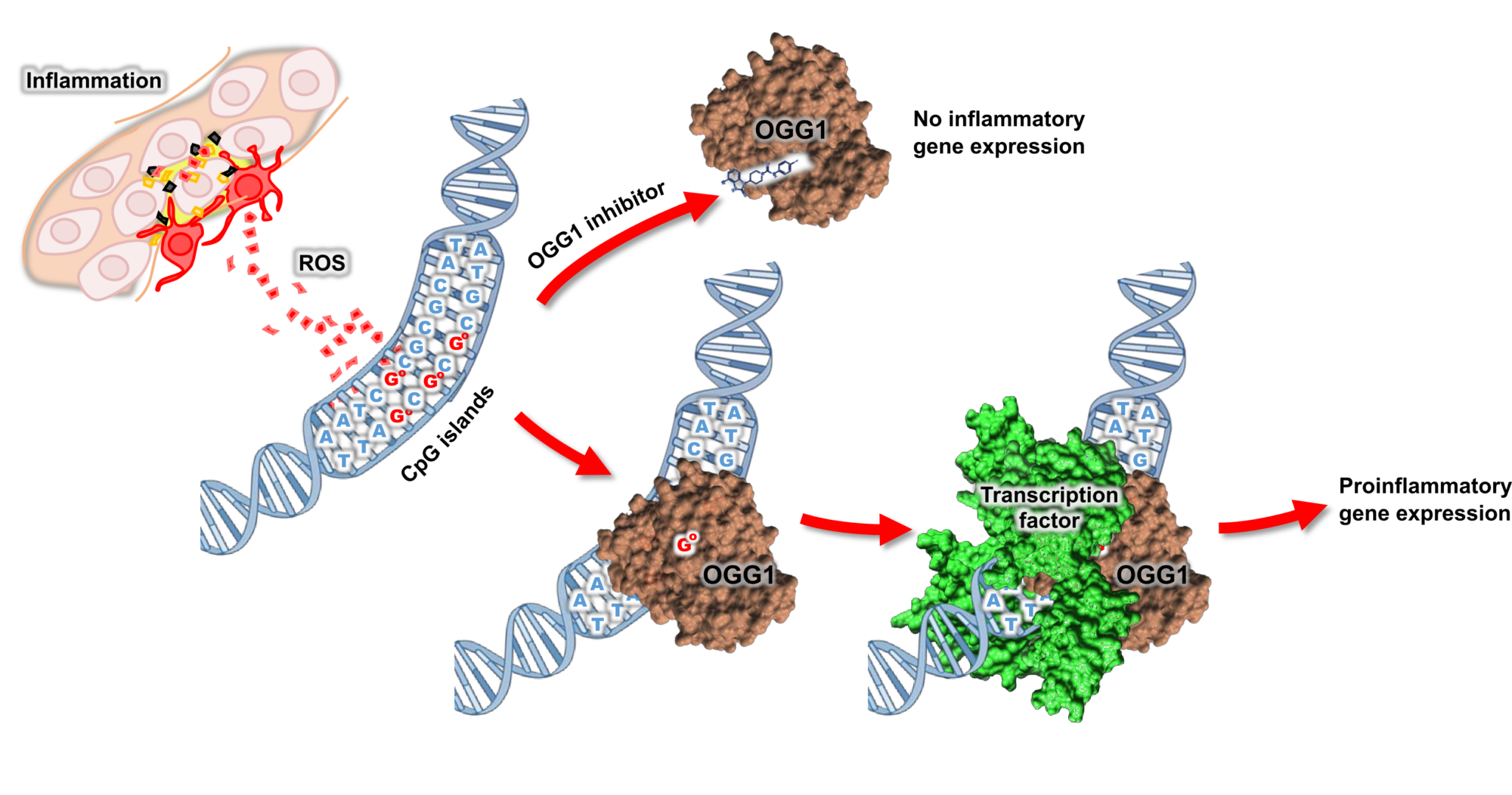
This is how the molecule TH5487 works. It “tricks” the repair enzyme into believing that it has already found the DNA it’s supposed to fix. This prevents the enzyme from trigging an inflammation. Illustration: SINTEF.
“I had previously been working exhaustively to measure activity levels of this class of enzyme using very laborious approaches,” Visnes explains. “But by developing a method that made it possible to determine enzyme activity using fluorescence (repaired DNA can be made to fluoresce), we were able to measure thousands of samples in the space of just a few hours.”
Visnes said that after examining 18,000 possible substances for properties that might fool the repair enzyme, the research team finally identified a substance that succeeded in deactivating OGG1. The process took a year.
Further development in the lab
Then began the laborious process of refining the substance so that it possessed all the properties needed to function in a living cell.
Over two years, the research team created roughly a thousand variations on the basic substance and were finally left with the promising drug candidate TH5487, named simply as a result of being made after variant TH5486.
TH5487 proved to have all of the three key properties that the researchers were looking for:
- It attached itself to the inflammation protein OGG1, inhibiting its activity and preventing it from bonding with DNA.
- It was able to deactivate OGG1 in living cells.
- It was very stable when injected into lab animals.
Healthier mice in Texas
The breakthrough came when researchers at the University of Texas tested the substance on mice suffering from serious cases of lung inflammation.
TH5487 rapidly and effectively prevented the lung cells from activating inflammation genes. As a result, immune cells did not register the developing infection and thus kept away from the lungs. The condition of the mice improved. The research team thus believes that they have discovered a new approach to suppressing inflammation that can be used instead of, or as a supplement to, existing treatments.
“The aim is to develop a drug that can work in people,” says Visnes. “This will be a long journey because it is expensive and the regulations are complex. But we believe that we’ve now discovered a piece in the puzzle that may have major significance for the treatment of everything from auto-immune diseases to blood poisoning.”
Visnes now wants to establish a separate biochemistry research group in Trondheim that would focus on DNA and drug development.